Nintedanib: ew treatment for malignant pleural mesothelioma
Introduction
A major change has been brought to thoracic oncology by the advent of biological therapies, and by “targeted” treatments in particular. These new approaches have changed the natural course of disease in patients with lung cancer, particularly those whose lung cancer is characterized by specific genetic mutations and rearrangements who may benefit from therapies that target these biomolecular alterations.
Among these drugs, molecules acting against multiple molecular targets have also been investigated, particularly Vargatef, which is a mult-target TKI that inhibits the VEGFR, FGFR and PDGFR receptors. It is currently approved in combination with docetaxel for advanced/metastatic lung adenocarcinoma after front-line chemotherapy. The scientific data for this treatment in lung cancer has shown benefit compared to standard chemotherapy alone in terms of progression-free survival (PFS) (4,0 vs 2,8) and overall survival (OS) (12,6 vs 10,3), with a reduction of 17% in the risk of death and a disease control rate of 60,2% (vs 44,0%). An analysis of the European population of the Lume-Lung 1 study showed a further increase in survival (13,4 vs 8,7).
This treatment was therefore considered as potentially useful also for MPM, an aggressive disease with a poor prognosis.
The purpose of this bibliographic review is to provide preliminary data on the use of nintedanib in mesothelioma.
Malignant pleural mesothelioma (MPM) is a cancerous disease that is no longer rare and unfortunately is very aggressive: if it is not treated, the average survival is 6-9 months.1-4
The standard first-line treatment for unresectable MPM is cisplatin and pemetrexed chemotherapy.5-9 Although this therapy helps increase median survival, it is still only reaches approximately one year so it is essential that new first-line treatments are developed.10-13
One approach to fulfil this goal is the investigation of antiangiogenics.14-22
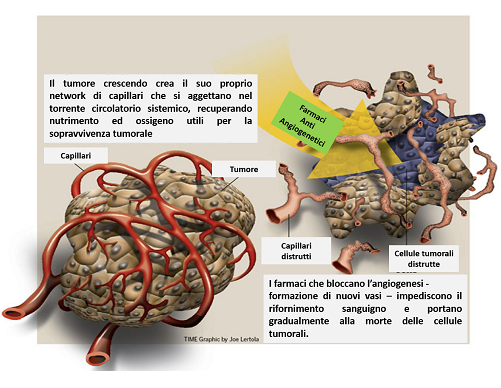
Specifically, the effectiveness of bevacizumab in combination with standard treatment as demonstrated in the MAPS study (Mesothelioma Avastin Cisplatin Pemetrexed Study), has led to renewed interest in inhibiting VEGF (vascular endothelial growth factor) as a therapeutic approach. In fact, many signaling molecules, which are involved in the angiogenesis regulation processes, are involved in both the pathogenesis and the prognosis of MPM.23,24 The VEGF pathway therefore plays a key role in regulating angiogenesis and consequently tumor growth, and is an important factor that can induce the proliferation of MPM cells.25 MPM patients also have high blood levels of VEGF, which is considered a negative prognostic factor.25
In the MAPS study, survival was shown to be significantly greater in MPM patients treated with cisplatin and pemetrexed plus bevacizumab, compared to those who received chemotherapy alone (18.8 months [confidence interval 95% (CI), 15.9-22.6] vs 16.1 months [95% CI 14.0-17.9]; hazard ratio [HR], 0.77 [95% CI 0.62-0.95]; P =.0167). (26) Up until then, no therapy had ever been shown to increase survival in MPM since the approval of pemetrexed by the US Food and Drug Administration in 2004. These results show that VEGF could be an effective approach as a therapeutic target.
One such drug is nintedanib, which acts on different signal transduction pathways that are involved in the pathogenesis of MPM. Specifically, the VEGF receptor is one of the targets of nintedanib and so this molecule is also considered an angiogenesis inhibitor.
The Phase III portion of the global Phase II/III LUME-Meso is evaluating the safety and efficacy of nintedanib in combination with pemetrexed and cisplatin in patients with unresectable epithelioid MPM.
Initially, this was a randomized, double-blind exploratory Phase II study, which was amended to include a confirmatory Phase III study, following an evaluation by an Internal Data Monitoring Committee after they had reviewed the Phase II results.
The Phase III study will enroll 450 patients not previously treated with chemotherapy, who will be randomized to receive pemetrexed/cisplatin on Day 1 and nintedanib or placebo from Day 2 to 21 for up to 6 cycles. Patients without progressive disease who are eligible to continue treatment in the study may receive maintenance treatment with nintedanib or placebo until disease progression or excessive toxicity. The primary endpoint of the study is progression-free survival (PFS); the key secondary endpoint is overall survival (OS). The study will also include interim analyses to ensure it is adequately powered for the statistical survival analyses. The study is currently enrolling patients.
The drug
Nintedanib is a tyrosine kinase inhibitor (TKI) that targets three growth factor receptors: the vascular endothelial growth factor receptor (VEGFR), the fibroblast growth factor receptor (FGFR), and the platelet-derived growth factor receptor (PDGFR), as well as other targets such as FLT3, RET, Abl and Src tyrosine-protein kinase signaling.27,28
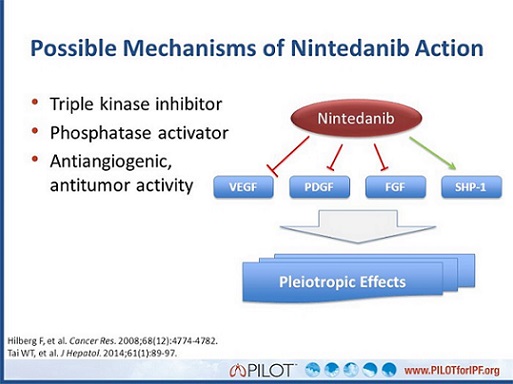
This drug is also indicated for idiopathic pulmonary fibrosis (IPF), which is a non-cancerous disease characterized by slow progression and fatal.29-31
It is associated with dyspnea, cough and reduced quality of life. Currently, the objectives of patient care include improving outcomes, obtained by slowing disease progression, increasing life expectancy and improving the quality of life.32-34 Timely and accurate diagnosis is important so that patients can be treated in the early stages of the disease and also so they can be considered for a lung transplant.35
The conditional recommendation of nintedanib for IPF is based on the results of the TOMORROW and INPULSIS studies, which showed that nintedanib 150 mg administered twice daily lowered the annual rate of change in FVC compared to patients who received placebo.36-41 The INPULSIS study results showed that nintedanib was consistently effective across the various subgroups defined by different characteristics such as age (<65 vs ≥65 years), race (Caucasian vs Asian), predicted FVC % (≤70% vs >70%; ≤80% vs >80%, <90% vs >90%), predicted DLCO % (>40% vs ≤40%), and several other diagnostic criteria (such as the presence of honeycombing on high-resolution CT and or confirmation of the presence of UIP by biopsy vs the potential presence of UIP with traction bronchiectasis detected by high-resolution CT, without biopsy evaluation).42-46
The TOMORROW and INPULSIS studies also showed that nintedanib reduced exacerbations and mortality due to IPF vs. placebo.47
Regarding the tolerability profile, adverse events occurred in more than 10% of patients treated with nintedanib. These adverse events included diarrhea, nausea, abdominal pain, vomiting, and raised liver enzymes, which occurred more frequently in patients receiving nintedanib than placebo.48,49 For the most part, the adverse events were managed by reducing the dose of the drug or discontinuing treatment.50 Results from INPULSIS_ON, the ongoing extension of the INPULSIS study, confirm the good tolerability profile of nintedanib and its effectiveness in lowering FVC for over three years.51
In oncology, nintedanib (BIBF 1120) in combination with docetaxel was approved by the European Medicines Agency (EMA) for use in the European Union and several other countries for the treatment of locally advanced, metastatic or locally recurrent NSCLC after first-line chemotherapy.52
It can also be given in combination with various anti-neoplastic treatments due to the efficacy and good safety profile it has shown when used for the treatment of different types of tumors.27
The ability of nintedanib to act on the three major pro-antiangiogenic signaling pathways (VEGF, PDGF and FGF) may offer greater clinical benefit to patients with unresectable MPM than that obtained with agents that target other known anti-angiogenic targets. Nintedanib also inhibits Src,27 a molecule that plays an important role in several neoplastic pathways and is involved in the pathogenesis of mesothelioma. Inhibition of Src has also been proposed as a therapeutic target for MPM.53 In preclinical studies, nintedanib reduced the growth and ability of MPM cell lines to metastasize and increased survival in an orthotopic xenograft model of MPM. It is therefore considered a valid candidate for the treatment of unresectable MPM.54
The study
LUME-Meso is a randomized, double-blind, placebo-controlled Phase II/III study.
The study compares the efficacy of nintedanib in combination with backbone pemetrexed+cisplatin chemotherapy followed by maintenance treatment with nintedanib, vs. placebo in combination with pemetrexed+cisplatin followed by placebo monotherapy in patients with unresectable MPM.
The study was initially an exploratory randomized, double-blind Phase II study only, but it was enlarged to include a confirmatory Phase III following the recommendation of an Internal Data Monitoring Committee after a review of the Phase II results.
After completing enrollment in the Phase II study, the results for the primary endpoint of PFS were presented.55 This led to nintedanib being granted Orphan Drug Designation by the US FDA on 12 December 2016. The Phase III study is currently enrolling and the data will be reviewed by an independent committee.
Study Purpose and Design and Treatment Regimen
The purpose of the study is to evaluate the tolerability and efficacy of backbone chemotherapy in combination with nintedanib followed by maintenance therapy with nintedanib, vs. backbone chemotherapy of cisplatin+pemetrexed in combination with placebo, followed by placebo monotherapy, as first-line treatment of unresectable MPM.
epitelioide e bifasica, è stato previsto nella fase III l'arruolamento di 450 pazienti, caratterizzati unicamente da MPM ad istologia epitelioide.
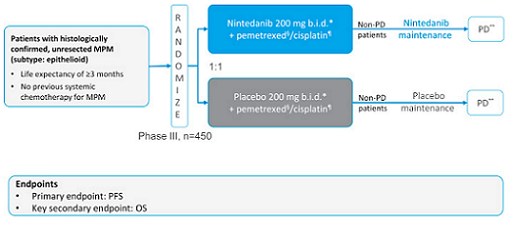
Figura 1. Disegno della fase III del trial LUME-Meso.∗Nintedanib è somministrato dal giorno 2 al 21; ¶Cisplaino 75 mg/m2 in infusione endovenosa. per 2 ore il giorno 1 di ciascun ciclo, della durata di 21 giorni, per un massimo di 6 cicli; §Pemetrexed 500 mg/m2 in infusione endovenosa in 10 minuti il giorno 1 di ciascun ciclo, della durata di 21 giorni, per un massimo di 6 cicli;∗∗Trattamento dopo la progressione è ammesso qualora sia atteso un vantaggio clinico.
Abbreviations: b.i.d. = due volte al giorno; I.V. = endovenosa; MPM = mesotelioma pleurico maligno; OS = sopravvivenza globale (overall survival); PD = Progressione di malattia; PFS = malattia libera da progressione (progression-free survival).
Patients are randomized 1:1 to receive pemetrexed (500 mg/m2)/cisplatin (75 mg/m2) on Day 1 for up to 6 cycles, in combination with nintedanib (200 mg twice per day) or placebo (twice per day) from Day 2 to Day 21. Patients will subsequently receive maintenance therapy with nintedanib or placebo until evidence of progressive disease (PD), the development of severe toxicity, withdrawal of consent or death. Patients who, in the opinion of the investigator, may derive a clinical benefit from continuing treatment after disease progression may continue treatment with nintedanib/placebo.
Based on the results of the Phase II study, which included patients with epithelioid and biphasic MPM histologies, the Phase III will enroll 450 patients with epithelioid MPM only.
Figure 1. Design of the Phase III LUME-Meso trial∗Nintedanib is administered from Day 2 to 21; ¶Cisplatin 75 mg/m2 intravenously for 2 hours on Day 1 of each cycle, for a duration of 21 days, for up to 6 cycles; §Pemetrexed 500 mg/m2 intravenously for 10 minutes on Day 1 of each cycle, for a duration of 21 days, for up to 6 cycles; &lowest;∗Treatment after progression is permitted if clinical benefit is anticipated.
Abbreviations: b.i.d. = twice daily; I.V. = intravenous; MPM = malignant pleural mesothelioma; OS = overall survival; PD = Progressive disease; PFS = progression-free survival.
Inclusion criteria
The study is conducted in accordance with the Helsinki Declaration and following approval by the Ethics Committee.
All patients must provide their informed consent in writing. The Phase III study is currently enrolling patients with histologically confirmed unresectable epithelioid MPM. Although patients eligible for radical resection or elective surgery (e.g., pleurectomy) are not eligible for enrollment, prior surgery, if performed at least 4 weeks before randomization, is permitted if the patient is fully healed and still has measurable disease.
Study Endpoint
The primary endpoint is PFS, while OS is the main secondary endpoint. Other secondary endpoints include overall response rate (ORR) and the percentage of patients with a complete or partial response, or stable disease control rate (DCR), as measured by modified RECIST Criteria.56 Another objective of the Phase III study includes evaluating the quality of life associated with health status as measured by the EuroQoL-5 self-evaluation questionnaire and the Lung Cancer Symptom Scale (LCSS-Meso) for mesothelioma.57,58
Biological samples will be tested by immunohistochemical or molecular genetic analysis to determine the value of markers such as mesothelin, merlin protein (produced by the NF2 gene) and protein 1 associated with BRCA1, as predictive or prognostic factors.
During the study, tolerability of the treatment will be monitored by evaluating variations in the laboratory parameters and the frequency and severity of adverse events in accordance with the CTCAE criteria (Common Terminology Criteria for Adverse Events version 4.03), established by National Cancer Institute (NCI). .59
Conclusion
As always, the main objective of the study is to increase survival and improve the quality of life.
The study of the new therapy aims to achieve these objectives, although the research requires time in order to validate the data before the results can be applied in clinical practice.
The Phase II/III LUME-Meso study will determine whether nintedanib in combination with the backbone of cisplatin+pemetrexed can provide clinical benefit to patients.
The Phase III study is currently underway, and eligible patients with unresectable MPM are being enrolled at sites in North and South America, Europe, Africa, Australia and Asia.
References
1. Baas, P. et al. Malignant pleural mesothelioma: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol 26 Suppl 5, v31-39 (2015).
2. Scherpereel, A. et al. Guidelines of the European Respiratory Society and the European Society of Thoracic Surgeons for the management of malignant pleural mesothelioma. Eur Respir J 35, 479-495 (2010).
3. Wagner, J. C., Sleggs, C. A. & Marchand, P. Diffuse pleural mesothelioma and asbestos exposure in the North Western Cape Province. Br J Ind Med 17, 260-271 (1960).
4. Steele, J. P. C. Prognostic factors for mesothelioma. Hematol Oncol Clin North Am 19, 1041-1052, vi (2005).
5. NCCN Guidelines. Malignant Pleural Mesothelioma Version 3.2016. (Available at:) https://www.ncbi.nlm.nih.gov/labs/articl.
6. van Meerbeeck, J. P., Scherpereel, A., Surmont, V. F. & Baas, P. Malignant pleural mesothelioma: the standard of care and challenges for future management. Crit Rev Oncol Hematol 78, 92-111 (2011).
7. Vogelzang, N. J. et al. Phase III study of pemetrexed in combination with cisplatin versus cisplatin alone in patients with malignant pleural mesothelioma. J Clin Oncol 21, 2636-2644 (2003).
8. Gelvez-Zapata, S. M., Gaffney, D., Scarci, M. & Coonar, A. S. What is the survival after surgery for localized malignant pleural mesothelioma? Interact Cardiovasc Thorac Surg 16, 533-537 (2013).
9. Ceresoli, G. L. et al. Phase II study of pemetrexed plus carboplatin in malignant pleural mesothelioma. J Clin Oncol 24, 1443-1448 (2006).
10. Dubey, S. et al. A phase II study of sorafenib in malignant mesothelioma: results of Cancer and Leukemia Group B 30307. J Thorac Oncol 5, 1655-1661 (2010).
11. Nowak, A. K. et al. A phase II study of intermittent sunitinib malate as second-line therapy in progressive malignant pleural mesothelioma. J Thorac Oncol 7, 1449-1456 (2012).
12. Buikhuisen, W. A. et al. Thalidomide versus active supportive care for maintenance in patients with malignant mesothelioma after first-line chemotherapy (NVALT 5): an open-label, multicentre, randomised phase 3 study. Lancet Oncol 14, 543-551 (2013).
13. Kindler, H. L. et al. Multicenter, double-blind, placebo-controlled, randomized phase II trial of gemcitabine/cisplatin plus bevacizumab or placebo in patients with malignant mesothelioma. J Clin Oncol 30, 2509-2515 (2012).
14. Ohta, Y. et al. VEGF and VEGF type C play an important role in angiogenesis and lymphangiogenesis in human malignant mesothelioma tumours. Br J Cancer 81, 54–61 (1999).
15. Jackman, D. M. et al. Erlotinib plus bevacizumab in previously treated patients with malignant pleural mesothelioma. Cancer 113, 808-814 (2008).
16. Dowell, J. E. et al. A multicenter phase II study of cisplatin, pemetrexed, and bevacizumab in patients with advanced malignant mesothelioma. Lung Cancer 77, 567-571 (2012).
17. Ceresoli, G. L. et al. Phase II study of pemetrexed and carboplatin plus bevacizumab as first-line therapy in malignant pleural mesothelioma. Br J Cancer 109, 552-558 (2013).
18. Reck, M. et al. Phase III trial of cisplatin plus gemcitabine with either placebo or bevacizumab as first-line therapy for nonsquamous non-small-cell lung cancer: AVAil. J Clin Oncol 27, 1227-1234 (2009).
19. Hurwitz, H. et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med 350, 2335-2342 (2004).
20. Giantonio, B. J. et al. Bevacizumab in combination with oxaliplatin, fluorouracil, and leucovorin (FOLFOX4) for previously treated metastatic colorectal cancer: results from the Eastern Cooperative Oncology Group Study E3200. J Clin Oncol 25, 1539-1544 (2007).
21. Zhu, X., Wu, S., Dahut, W. L. & Parikh, C. R. Risks of proteinuria and hypertension with bevacizumab, an antibody against vascular endothelial growth factor: systematic review and meta-analysis. Am J Kidney Dis 49, 186-193 (2007).
22. Gray, R., Bhattacharya, S., Bowden, C., Miller, K. & Comis, R. L. Independent review of E2100: a phase III trial of bevacizumab plus paclitaxel versus paclitaxel in women with metastatic breast cancer. J Clin Oncol 27, 4966-4972 (2009).
23. Strizzi, L. et al. Vascular endothelial growth factor is an autocrine growth factor in human malignant mesothelioma. J Pathol 193, 468-475 (2001).
24. Garland, L. L. et al. Phase II study of cediranib in patients with malignant pleural mesothelioma: SWOG S0509. J Thorac Oncol 6, 1938-1945 (2011).
25. Tsao, A. S. et al. Inhibition of c-Src expression and activation in malignant pleural mesothelioma tissues leads to apoptosis, cell cycle arrest, and decreased migration and invasion. Mol Cancer Ther 6, 1962-1972 (2007).
26. Zalcman, G. et al. Bevacizumab for newly diagnosed pleural mesothelioma in the Mesothelioma Avastin Cisplatin Pemetrexed Study (MAPS): a randomised, controlled, open-label, phase 3 trial. Lancet 387, 1405-1414 (2016).
27. Roth, G. J. et al. Nintedanib: from discovery to the clinic. J Med Chem 58, 1053-1063 (2015).
28. Stinchcombe, T. E. Novel agents in development for advanced non-small cell lung cancer. Ther Adv Med Oncol 6, 240-253 (2014).
29. Buendia-Roldan, I., Mejia, M., Navarro, C. & Selman, M. Idiopathic pulmonary fibrosis: Clinical behavior and aging associated comorbidities. Respir Med 129, 46-52 (2017).
30. Raghu, G. & Richeldi, L. Current approaches to the management of idiopathic pulmonary fibrosis. Respir Med 129, 24-30 (2017).
31. Hewitt, R. J. & Molyneaux, P. L. The respiratory microbiome in idiopathic pulmonary fibrosis. Ann Transl Med 5, 250 (2017).
32. Koo, S.-M. & Uh, S.-T. Treatment of connective tissue disease-associated interstitial lung disease: the pulmonologist’s point of view. Korean J Intern Med 32, 600–610 (2017).
33. Johannson, K. A. et al. Antacid therapy in idiopathic pulmonary fibrosis: more questions than answers? Lancet Respir Med 5, 591-598 (2017).
34. Chioma, O. S. & Drake, W. P. Role of Microbial Agents in Pulmonary Fibrosis. Yale J Biol Med 90, 219-227 (2017).
35. Aiello, M. et al. The earlier, the better: Impact of early diagnosis on clinical outcome in idiopathic pulmonary fibrosis. Pulm Pharmacol Ther 44, 7-15 (2017).
36. Fukihara, J. & Kondoh, Y. Nintedanib (OFEV) in the treatment of idiopathic pulmonary fibrosis. Expert Rev Respir Med 10, 1247-1254 (2016).
37. Inomata, M., Nishioka, Y. & Azuma, A. Nintedanib: evidence for its therapeutic potential in idiopathic pulmonary fibrosis. Core Evid 10, 89-98 (2015).
38. Mazzei, M. E., Richeldi, L. & Collard, H. R. Nintedanib in the treatment of idiopathic pulmonary fibrosis. Ther Adv Respir Dis 9, 121-129 (2015).
39. Richeldi, L. et al. Efficacy of a tyrosine kinase inhibitor in idiopathic pulmonary fibrosis. N Engl J Med 365, 1079-1087 (2011).
40. Richeldi, L. et al. Efficacy and safety of nintedanib in idiopathic pulmonary fibrosis. N Engl J Med 370, 2071-2082 (2014).
41. Woodcock, H. V., Molyneaux, P. L. & Maher, T. M. Reducing lung function decline in patients with idiopathic pulmonary fibrosis: potential of nintedanib. Drug Des Devel Ther 7, 503-510 (2013).
42. Costabel, U. et al. Efficacy of Nintedanib in Idiopathic Pulmonary Fibrosis across Prespecified Subgroups in INPULSIS. Am J Respir Crit Care Med 193, 178-185 (2016).
43. Kolb, M. et al. Nintedanib in patients with idiopathic pulmonary fibrosis and preserved lung volume. Thorax 72, 340-346 (2017).
44. Raghu, G. et al. Effect of Nintedanib in Subgroups of Idiopathic Pulmonary Fibrosis by Diagnostic Criteria. Am J Respir Crit Care Med 195, 78-85 (2017).
45. T.M. Maher, Effect of baseline FVC on lung function decline with nintedanib in patients with IPF Eur. Respir. J., Suppl.
46. T.M. Maher, No effect of baseline diffusing capacity of lung for carbon monoxide on benefit of nintedanib Eur. Respir. J.
47. Richeldi, L. et al. Nintedanib in patients with idiopathic pulmonary fibrosis: Combined evidence from the TOMORROW and INPULSIS((R)) trials. Respir Med 113, 74-79 (2016).
48. Boehringer Ingelheim Pharmaceuticals, Inc http://bidocs.boehringeringelheim.com/BIWebAccess/ViewServlet.ser?docBase=ren.
49. Boehringer Ingelheim International GmbH http://products.boehringer-ingelheim.com/OFEV/sites/default/files/OFEV_SmPC_2016.
50. Corte, T. et al. Safety, tolerability and appropriate use of nintedanib in idiopathic pulmonary fibrosis. Respir Res 16, 116 (2015).
51. Crestani, Long-term treatment with nintedanib in patients with IPF: an update from INPULSIS®-ON Eur. Respir. J., 48 (Su.
52. Reck, M. et al. Docetaxel plus nintedanib versus docetaxel plus placebo in patients with previously treated non-small-cell lung cancer (LUME-Lung 1): a phase 3, double-blind, randomised controlled trial. Lancet Oncol 15, 143-155 (2014).
53. Menges, C. W. et al. A Phosphotyrosine Proteomic Screen Identifies Multiple Tyrosine Kinase Signaling Pathways Aberrantly Activated in Malignant Mesothelioma. Genes Cancer 1, 493-505 (2010).
54. Laszlo V, Ozsar J, Klikovits T, et al. Preclinical investigation of the therapeutic potential of nintedanib in malignant.
55. Grosso, N. Steele, S. Novello, et al. OA22.02 Nintedanib plus pemetrexed/cisplatin in patients with MPM: phase II findi.
56. Byrne, M. J. & Nowak, A. K. Modified RECIST criteria for assessment of response in malignant pleural mesothelioma. Ann Oncol 15, 257-260 (2004).
57. Trippoli, S., Vaiani, M., Lucioni, C. & Messori, A. Quality of life and utility in patients with non-small cell lung cancer. Quality-of-life Study Group of the Master 2 Project in Pharmacoeconomics. Pharmacoeconomics 19, 855-863 (2001).
58. Hollen, P. J., Gralla, R. J., Liepa, A. M., Symanowski, J. T. & Rusthoven, J. J. Measuring quality of life in patients with pleural mesothelioma using a modified version of the Lung Cancer Symptom Scale (LCSS): psychometric properties of the. Support Care Cancer 14, 11-21 (2006).
59. Elman, S. A., Ware, J. H., Gottlieb, A. B. & Merola, J. F. Adaptive Clinical Trial Design: An Overview and Potential Applications in Dermatology. J Invest Dermatol 136, 1325-1329 (2016).
